Post-nasal drip: fast fixes, real causes, and when to get help
That constant tickle or mucus pooling at the back of your throat? That’s post-nasal drip. It’s annoying, makes you clear your throat a lot, and can ruin sleep. The good news: most cases are easy to treat once you know the cause.
What causes it and how to tell
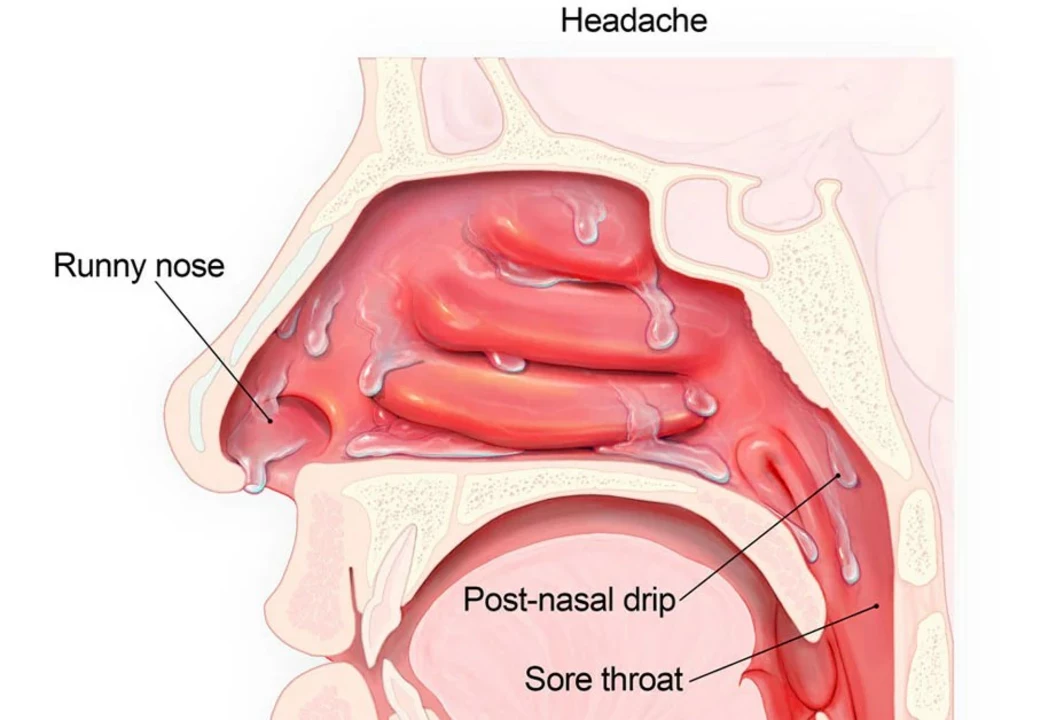
Post-nasal drip happens when your nose and sinuses produce extra mucus that runs down the throat. Common triggers are colds, seasonal allergies, sinus infections, and dry indoor air. Less common causes include acid reflux, certain medications, and structural issues like a deviated septum. If the mucus is thin and watery, think allergy or cold; thick, discolored mucus plus facial pressure often points to sinus infection.
Simple clues help you spot the cause: itchy eyes and sneezing usually mean allergies; fever and sore throat lean toward a viral infection; persistent green mucus and facial pain for more than 10 days could mean bacterial sinusitis.
Simple home treatments that actually work
Start with safe, low-effort fixes: keep drinking water to thin mucus, use a humidifier at night, and sleep with your head slightly elevated. Saline nasal rinses (neti pot or squeeze bottle) clear mucus well—only use distilled, sterile, or previously boiled and cooled water. Do saline rinses once or twice daily until you feel better.
Over-the-counter options can help too. Non-drowsy antihistamines like cetirizine or loratadine ease allergy-related drip. Nasal steroid sprays (fluticasone, budesonide) reduce inflammation when used daily for a few days. Short-term oral decongestants or topical nasal decongestant sprays can relieve congestion, but avoid nasal sprays for more than 3 days to prevent rebound congestion. If you have high blood pressure or heart disease, check with your doctor before using decongestants.
Steam inhalation (hot shower or bowl of hot water with a towel over your head) can loosen mucus for short relief. For babies and toddlers, use saline drops and a bulb syringe rather than sprays.
If reflux seems to trigger your drip (worse after meals, with heartburn), try eating smaller meals, avoid lying down right after eating, and cut back on spicy or fatty foods. Talk to your provider if reflux symptoms are frequent.
When over-the-counter measures don’t help after a week, or symptoms get worse, it’s time to see a clinician. They’ll do a nasal exam and may recommend allergy testing, prescription nasal steroids, antibiotics only if a bacterial infection is likely, or referral to an ENT specialist for persistent problems. Imaging or nasal endoscopy is rarely needed but useful for chronic or unclear cases.
If you have high fever, severe facial pain, trouble breathing, blood in mucus, or symptoms lasting more than 10–14 days despite treatment, seek medical care promptly. Those signs can mean a bacterial infection or another issue that needs prescription treatment.
Small changes—consistent saline rinses, a humidifier, and the right OTC choice—fix most cases. If you keep getting post-nasal drip, jot down when it happens, what makes it worse, and any triggers like pets or smoke. That info speeds up diagnosis and gets you back to normal sooner.
- May 27, 2023
- SkyCaddie Fixer
- 8 Comments
Bromhexine: A Solution for Post-Nasal Drip and Persistent Cough
As someone who has suffered from post-nasal drip and persistent cough, I've recently discovered Bromhexine as a potential solution. This medication works by thinning and loosening mucus, making it easier to expel from the respiratory tract. I've found it to be quite effective in relieving my cough and clearing out any excess mucus. It's important to remember that it's always best to consult a doctor before trying out any new medication. Bromhexine has definitely improved my quality of life and I wanted to share my experience with others who may be struggling with similar issues.
