Causes: What Triggers Health Problems and How to Spot Them
This tag collects plain answers about why things go wrong with your health. You’ll find articles that explain causes behind symptoms, medication reactions, and disease risks. Use these posts to get a clear idea of what might be triggering your issue and what to ask your doctor next.
When you read a piece here, look for three things: the direct cause (like an infection or a drug), contributing factors (sleep, diet, stress), and warning signs that need urgent care. Most pages break that down, so you can quickly compare possible reasons instead of guessing.
Quick checklist to identify likely causes
Start simple. Ask: When did the problem begin? Did you start a new medicine, change diet, or get sick recently? If symptoms started after a new drug, the medication could be the cause. If they began after travel or exposure, think infection or environment.
Next, match symptoms to common sources. Fever, chills, and body aches usually point to infection. Sudden chest pain or trouble breathing needs emergency care. Long-term fatigue, weight change, or mood shifts often come from sleep, hormones, or chronic conditions. Don’t ignore patterns: daily headaches that flare after screen time point to posture and eye strain; heartburn after big meals suggests reflux.
Look at risk factors you can change. Smoking, heavy drinking, poor sleep, and low activity are common drivers of problems. Some causes are less obvious: side effects from cholesterol or blood pressure meds can show up as sleep trouble or muscle pain, and some supplements interact with prescriptions. Our posts highlight these links so you can spot them fast.
When to act and what to tell your clinician
If you suspect a cause you can fix—stop a supplement, adjust sleep, reduce alcohol—try small changes and track results for a week or two. Keep a short log of symptoms, timing, and anything new you did. That record makes appointments far more useful.
Call your provider right away if you have chest pain, fainting, severe shortness of breath, sudden weakness, high fever, or severe allergic reactions. For non-urgent concerns, bring your symptom log, a list of meds and supplements, recent medical tests, and clear notes on when things began. Ask your clinician whether testing or a trial change in treatment makes sense.
Use this tag as a starting point—not a final diagnosis. Articles here give practical causes and red flags, point to likely tests, and show when a medication or lifestyle factor may be the reason. Read with a clear goal: find plausible causes, test simple fixes, and know when to get medical help.
- May 12, 2023
- SkyCaddie Fixer
- 16 Comments
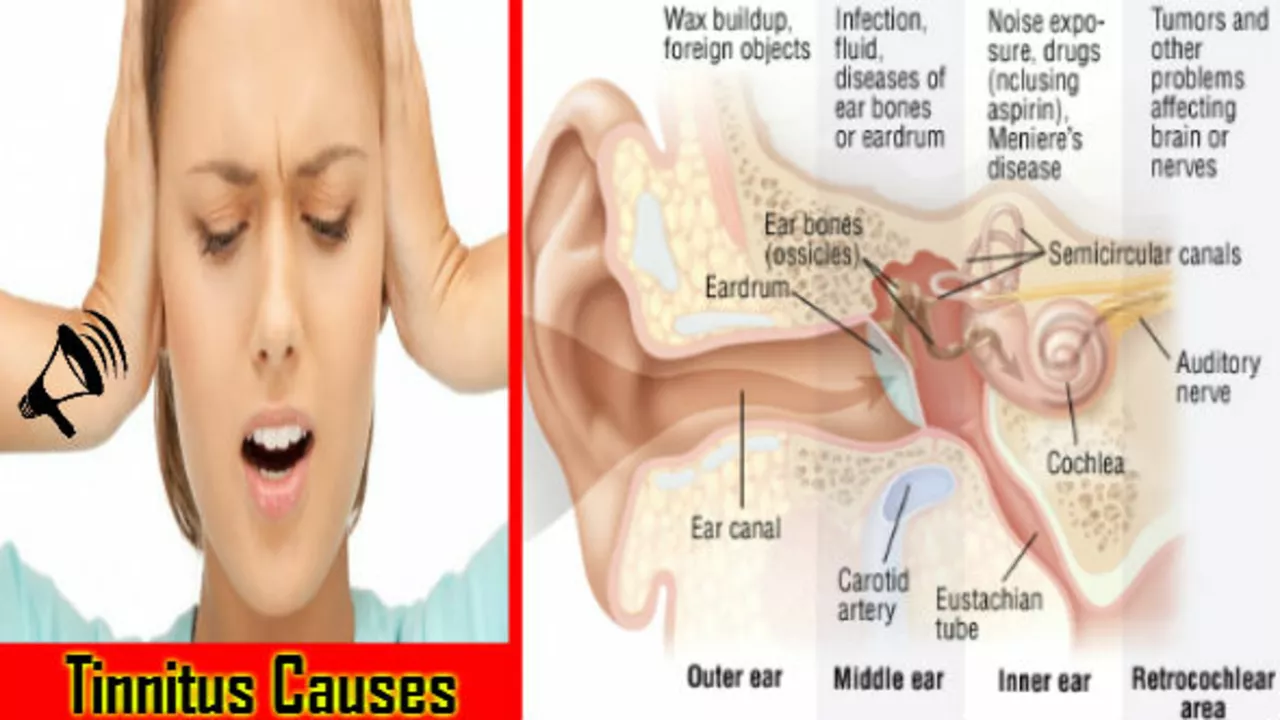
The Connection Between Propranolol and Tinnitus: Causes and Solutions
As a sufferer of tinnitus, I recently came across some interesting information about the connection between Propranolol and this frustrating condition. Propranolol is a beta-blocker commonly used to treat high blood pressure and anxiety. However, it has been found that it can sometimes cause or worsen tinnitus in certain individuals. Thankfully, there are alternative medications and treatments available if you're affected by this side effect. I'll be exploring these options in my upcoming posts, hoping to provide relief for those struggling with tinnitus.
