The good news is that these mistakes are almost entirely preventable. If you move away from "guessing" and start using standardized tools and a few simple double-checks, you can virtually eliminate the risk of a dosing blunder. Here is exactly how to handle liquid meds safely at home and what to look for in a professional healthcare setting.
Stop Using Kitchen Spoons Immediately
If you are still using a teaspoon or tablespoon from your silverware drawer, you are playing a dangerous game. Household spoons are not measuring devices; they are eating utensils. Their volumes vary wildly from one brand to another. According to the NIH, kitchen spoons have a staggering 62% accuracy rate for common doses, compared to the near-perfect precision of professional tools.
The wrong-dose errors is a type of medication error where the volume of a liquid pharmaceutical administered differs from the prescribed amount. To stop this, you need to stick exclusively to metric units-specifically milliliters (mL). The World Health Organization notes that removing non-metric units (like "teaspoons") is the single most effective way to stop these errors, potentially preventing 33% of all dosing mistakes.
The Gold Standard: Oral Syringes
Not all measuring tools are created equal. While many pharmacies still hand out those little plastic dosing cups, they are surprisingly unreliable. In a multi-site study published in Academic Emergency Medicine, dosing cups showed an error rate of 41.1% for doses under 5 mL. In contrast, Oral Syringes-which are plastic piston-driven devices used to deliver precise volumes of liquid medication into the mouth-had an error rate of only 8.2%.
For the best accuracy, follow these guidelines based on the dose size:
- Doses under 1 mL: Use a syringe with 0.1 mL graduations.
- Doses between 1 and 5 mL: Use a syringe with 0.5 mL graduations.
| Tool Type | Accuracy Rate (2.5 mL Dose) | Primary Risk |
|---|---|---|
| Oral Syringe | 94% | Minimal/None |
| Dosing Cup | 76% | Surface tension/spillage |
| Household Spoon | 62% | Non-standard volume |
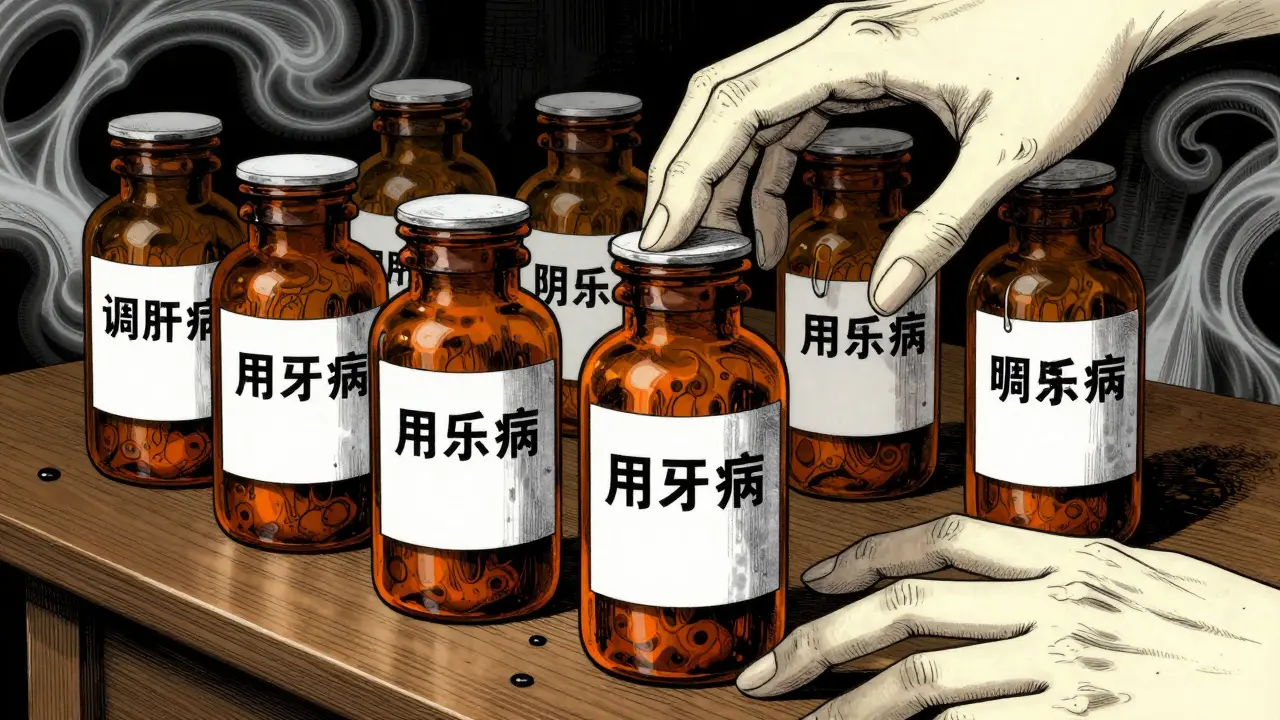
Spotting and Avoiding "Look-Alike" Mistakes
Ever noticed how two different medications can come in almost identical amber bottles? This is a major trigger for Dispensing Errors, which occur when the pharmacy provides the wrong drug or the wrong strength. When the packaging looks the same, it is incredibly easy to grab the wrong bottle, especially when you're tired or rushing.
To prevent this, look for labels that meet the ANSI Z535.4-2011 safety standards. High-quality pharmacies use bold, high-contrast labels like "FOR ORAL USE ONLY" to distinguish oral liquids from other medications. If you are a caregiver, a great pro tip is to mark your bottles with a permanent marker or use colorful rubber bands to differentiate between medications that look the same.
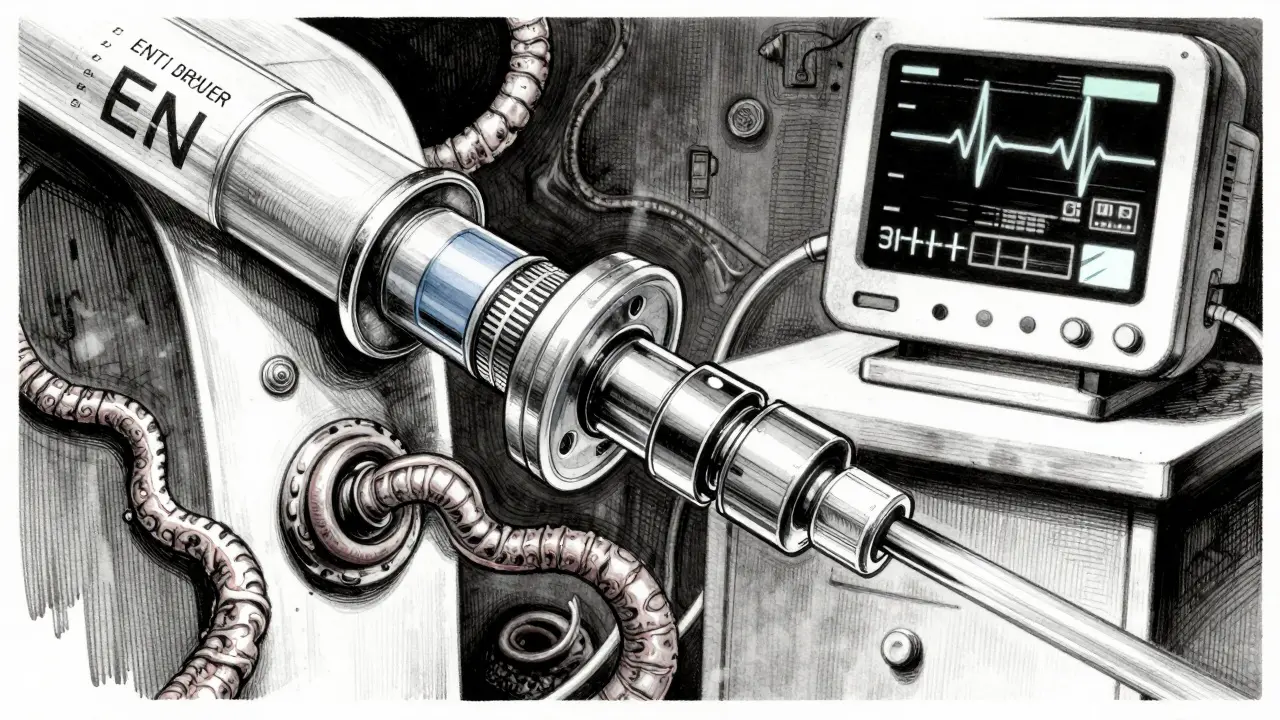
Safety in the Hospital: The ENFit System
If you have a loved one in a hospital, you might notice a specific type of connector on their feeding tubes. This is likely the ENFit system, which is a standardized enteral connection system designed to prevent the accidental administration of tube feedings or medications into intravenous (IV) lines. Before this, connectors were often compatible, meaning a nurse could accidentally push a liquid medication into a vein instead of the stomach-a potentially fatal mistake.
The ENFit system uses geometrically incompatible connectors. This means the plug simply won't fit into an IV port. Hospitals that have fully implemented this ISO 80369-3 standard have seen wrong-route administration errors drop by a staggering 98%. It's a clear example of how a physical design change can solve a human error problem.
Double-Checking the Prescription Process
Most errors start long before the medicine reaches the patient. About 38% of errors happen during the prescribing phase. This is often due to manual calculation mistakes when a doctor determines a dose based on a child's weight. This is why Computerized Physician Order Entry (CPOE) is such a game-changer. CPOE is a software system that allows providers to enter medication orders electronically instead of handwriting them.
Modern CPOE systems include clinical decision support that acts like a safety net. If a doctor accidentally types a dose that is 20% outside the standard weight-based parameter, the system flags it immediately. These digital checks have been shown to reduce pediatric liquid medication errors by 58%. When you pick up a prescription, don't be afraid to ask the pharmacist: "Does this dose match the patient's weight?" and "Can I have an oral syringe instead of a cup?"
A Quick Safety Checklist for Caregivers
To keep your home environment safe, treat every dose like a professional medical procedure. Follow these steps every single time:
- Verify the Device: Throw away the spoons. Use only a metric oral syringe.
- Check the Label: Read the medication name and concentration (e.g., 250mg/5mL) twice.
- Eye-Level Pour: Always measure liquid at eye level on a flat surface to avoid parallax errors.
- Confirm the Volume: Ensure the plunger is exactly on the line for the required mL.
- Double-Verify: If possible, have another adult check the dose before administration.
Why are oral syringes better than dosing cups?
Oral syringes are far more accurate, especially for small doses under 5 mL. They eliminate the liquid that sticks to the sides of a cup and allow for much more precise graduations (down to 0.1 mL), whereas cups often have confusing markings and higher spillage rates.
What should I do if the pharmacist didn't give me a measuring tool?
Do not use a kitchen spoon. Call the pharmacy back or visit them to request a metric oral syringe. Most pharmacies provide these for free or at a very low cost, and it is the only safe way to ensure the patient receives the correct dose.
What is a "look-alike" medication error?
This happens when two different medications have very similar packaging, bottle shapes, or label colors, leading a caregiver to administer the wrong medication entirely. This can be prevented by using high-contrast labels and adding personal identifiers (like colored tape) to the bottles.
Is the ENFit system used for all liquid medicines?
No, the ENFit system is specifically designed for enteral (feeding tube) administration in clinical settings to prevent medications from being accidentally injected into an IV line. It is not used for standard oral medications taken by mouth.
How can I tell if a dose was wrong?
Signs of a wrong dose vary. An underdose may lead to treatment failure (e.g., a fever not breaking), while an overdose can cause toxicity, extreme drowsiness, or respiratory distress. If you suspect a dosing error, contact a poison control center or your doctor immediately.

